Gum Disease Stages: Early Warning Signs You Should Never Ignore
You spit out a little pink in the sink after brushing and tell yourself it's nothing. Maybe you pressed too hard. Maybe it happens to everyone. But if your gums are bleeding, swollen, or pulling away from your teeth, your mouth may be sending you one of the clearest early signs of gum disease you'll ever get — and the earlier you recognize it, the easier it is to reverse.
Gum disease affects an estimated 47% of adults over age 30 in the United States, according to the Centers for Disease Control and Prevention (CDC). Yet the majority of cases go undiagnosed and untreated in their early stages simply because the symptoms seem minor. This guide walks through each of the four stages of gum disease, what you'll actually see and feel at each stage, what causes the disease to worsen, and what you can do to stop it.
What Is Gum Disease?
Gum disease — clinically called periodontal disease — is a bacterial infection of the structures that support your teeth: the gums, the ligaments that anchor teeth to bone, and the jawbone itself. It starts at the gumline, where dental plaque (a sticky film of bacteria) accumulates if not removed daily. When plaque hardens into tartar and bacteria multiply below the gumline, the body's immune response triggers inflammation — and that inflammation, left unchecked, slowly destroys tissue and bone.
The important thing to understand is that gum disease is a progressive condition. It moves through distinct stages, each more serious than the last. The earliest stage — gingivitis — is fully reversible. The later stages are not. That distinction is why recognizing gingivitis symptoms early is so important.
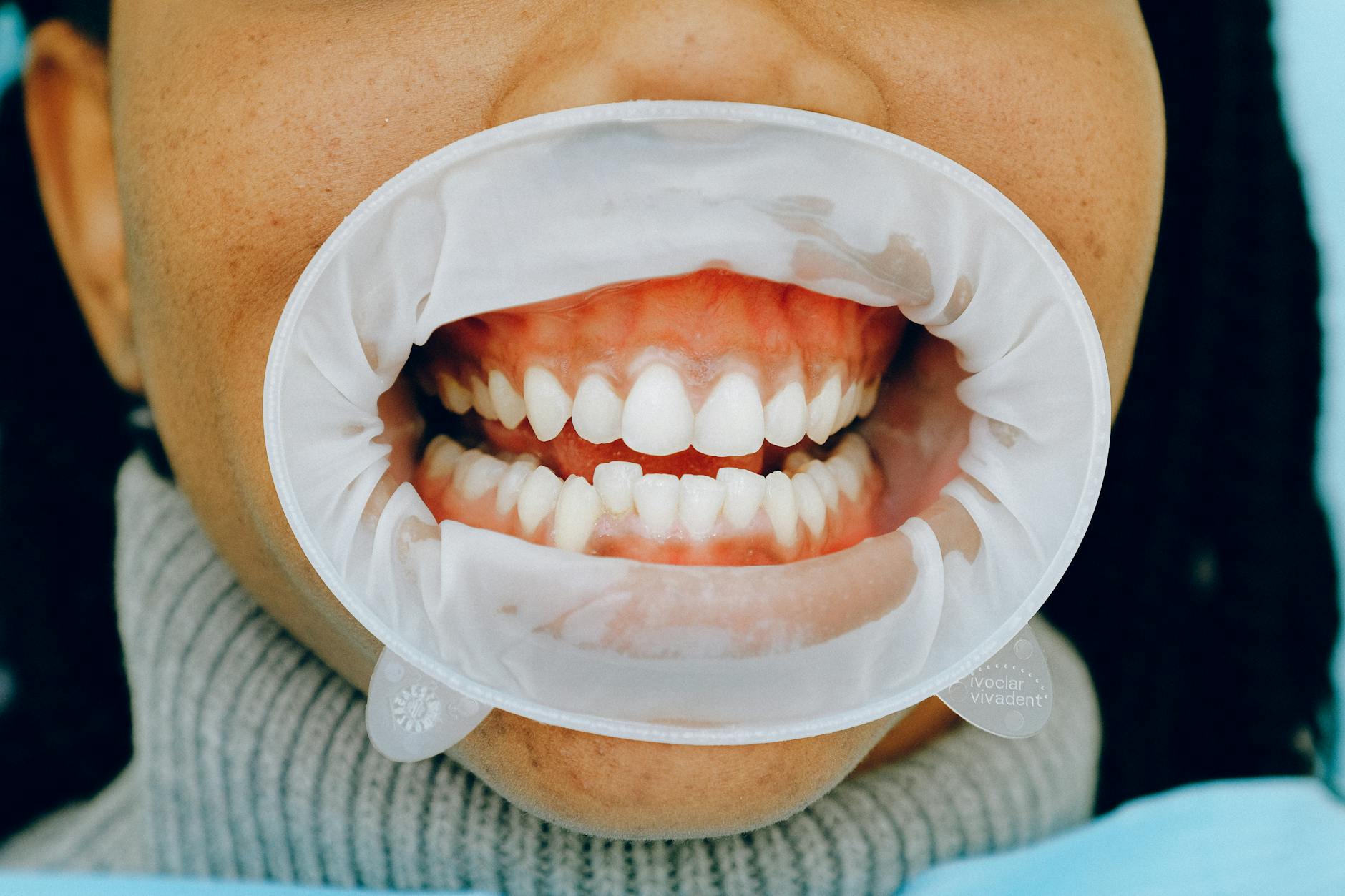
Stage 1: Healthy Gums — What Normal Looks Like
Before covering the stages of disease, it helps to know what healthy gums look like so you have a baseline for comparison. Healthy gums are:
- Firm — they don't feel puffy, soft, or tender to the touch
- Pale pink — a consistent coral or salmon pink (darker in people with more melanin, but uniform in color)
- Tightly fitted around each tooth — no gaps or pockets visible at the gumline
- Non-bleeding — brushing and flossing should not cause bleeding
- Odor-free — healthy mouths do not produce persistent bad breath
If your gums currently match this description, your job is maintenance: brush twice daily for two minutes with a soft-bristled brush, floss once daily, and get a professional cleaning every six months. That's genuinely all it takes for most people to stay at this stage indefinitely.
Stage 2: Gingivitis — The Reversible Stage
Gingivitis is the earliest stage of gum disease, and critically, it is the only stage that is completely reversible. At this point, bacterial infection and inflammation are confined entirely to the gum tissue itself — the bone and deeper supporting structures have not yet been affected.
Gingivitis Symptoms to Watch For
- Bleeding when brushing or flossing — the most common and earliest warning. Healthy gums do not bleed; bleeding is always a sign of inflammation.
- Redness and swelling — gums shift from pale pink to a deeper red or purplish hue and may look puffy along the margins
- Tenderness — gums may feel sensitive to touch or during eating
- Persistent bad breath (halitosis) — caused by bacteria metabolizing proteins below the gumline
- Gums that look slightly "pulled" from teeth — mild separation can occur even at this early stage
What makes gingivitis deceptive is that it is often painless. Many people with active gingivitis feel nothing unusual — they only notice the blood on the toothbrush or a slightly different appearance in the mirror. The American Dental Association (ADA) notes that because gingivitis doesn't hurt, it is frequently ignored until it advances.
The good news: gingivitis can be completely reversed with improved oral hygiene and a professional dental cleaning to remove tartar buildup. Studies published in the Journal of Clinical Periodontology consistently show that patients who commit to proper brushing, daily flossing, and professional cleanings can achieve full gum health resolution within four to eight weeks.
Stage 3: Mild to Moderate Periodontitis — When Damage Begins
If gingivitis is not treated, the infection progresses below the gumline and begins destroying the bone and connective tissue that hold teeth in place. This is periodontitis — and unlike gingivitis, the damage it causes is permanent. You can stop further destruction, but you cannot undo what has already been lost without surgical intervention.
At this stage, the space between the tooth and gum (the "pocket") deepens as tissue detaches. Dentists measure pocket depth with a probe during exams — a healthy pocket is 1–3mm; mild to moderate periodontitis typically produces pockets of 4–6mm. That extra depth creates an anaerobic environment where dangerous bacteria thrive beyond the reach of a toothbrush.
Periodontitis Warning Signs at This Stage
- Visibly receding gums — teeth begin to look longer as the gumline pulls back
- Increased tooth sensitivity — exposed root surfaces react to hot, cold, and sweet foods
- Persistent bad breath that doesn't resolve with brushing
- Gums that bleed more easily and heavily — sometimes spontaneously, not just during brushing
- Mild tooth looseness — bone loss begins to reduce the support structure for teeth
- Pus between teeth and gums — a sign of active bacterial infection
- A change in bite — teeth may shift subtly as supporting structures weaken

Treatment at this stage moves beyond a standard cleaning. A dentist or periodontist will typically perform scaling and root planing — a deep-cleaning procedure done under local anesthesia that removes tartar and bacteria from below the gumline and smooths the root surfaces to discourage future bacterial adhesion. Multiple follow-up visits and ongoing maintenance cleanings (typically every three to four months rather than six) become necessary.
Stage 4: Advanced Periodontitis — Severe and Potentially Tooth-Threatening
Advanced periodontitis represents significant bone and tissue loss. Pockets deepen to 7mm or more. The teeth's support structure has been substantially compromised, and without aggressive treatment, tooth loss becomes likely. The CDC reports that periodontitis warning signs at this stage are unmistakable — yet many patients still delay seeking care.
Advanced Periodontitis Warning Signs
- Severely receding gums — roots are extensively exposed, making teeth look dramatically elongated
- Significant tooth looseness or shifting — teeth may move when you push them with your tongue
- Tooth loss — in the most severe cases, teeth fall out or require extraction
- Severe, chronic bad breath — not relieved by any oral hygiene measure
- Bite changes and difficulty chewing — drifting teeth alter how upper and lower teeth meet
- Jaw pain — deep bone infection can cause aching discomfort in the jaw
- Abscesses — pockets of pus that form at the root tips or gumline
Treatment at this stage often requires surgical intervention — including flap surgery (lifting the gum tissue to allow deeper cleaning and bone reshaping), bone grafting to replace lost bone, or guided tissue regeneration. Some patients require a combination of these procedures. The goal is to arrest further progression; regenerating what has already been lost is only partially possible even with modern techniques.
Beyond the mouth, advanced periodontitis carries systemic implications. Research published in the Journal of the American Heart Association and multiple meta-analyses links advanced gum disease to increased risk of cardiovascular disease, type 2 diabetes complications, adverse pregnancy outcomes, and respiratory disease. The chronic inflammation driven by periodontal bacteria appears to contribute to inflammatory processes throughout the body.
What Causes Gum Disease to Progress?
Understanding the risk factors that accelerate progression is as important as recognizing the symptoms. The stages of gum disease don't advance at the same rate in every person — some people with poor oral hygiene develop only mild gingivitis while others progress rapidly to periodontitis. Several factors influence this:
Modifiable Risk Factors
- Poor oral hygiene — infrequent brushing and skipping flossing allows plaque to accumulate and harden into tartar
- Smoking and tobacco use — tobacco is one of the strongest risk factors for periodontitis; it impairs immune response and reduces blood flow to gum tissue, masking bleeding symptoms while accelerating bone loss
- Uncontrolled diabetes — high blood glucose impairs the body's ability to fight infection, making diabetics two to three times more likely to develop periodontitis
- Stress — chronic stress elevates cortisol, which suppresses immune function and increases susceptibility to infection
- Certain medications — drugs that reduce saliva flow (antihistamines, antidepressants, blood pressure medications) increase risk, as do some immunosuppressants and anticonvulsants that cause gum overgrowth
- Poor nutrition — vitamin C deficiency in particular directly impairs gum tissue integrity
Non-Modifiable Risk Factors
- Genetics — research suggests up to 30% of the population may have a genetic predisposition to more aggressive gum disease regardless of oral hygiene habits
- Age — prevalence increases sharply with age; 70% of adults over 65 have some form of periodontitis
- Hormonal changes — pregnancy, puberty, and menopause all create periods of heightened gum sensitivity and inflammatory response
How to Prevent Gum Disease: Evidence-Based Habits
The research on how to prevent gum disease is remarkably consistent. Unlike many areas of health where the science is contested, the fundamentals of gum disease prevention are well-established and straightforward. The challenge is not knowing what to do — it is doing it consistently.
Daily Oral Hygiene Essentials
- Brush for two full minutes, twice a day — use a soft-bristled brush and hold it at a 45-degree angle to the gumline to clean below the gum margin. Electric toothbrushes have been shown in clinical studies to remove up to 21% more plaque than manual brushes.
- Floss once daily — this is non-negotiable for gum health. Flossing removes plaque from between teeth and below the gumline in areas a brush cannot reach. Interdental brushes or water flossers are acceptable alternatives for those who find traditional floss difficult.
- Consider an antiseptic mouthwash — chlorhexidine mouthwashes (available by prescription) are among the most effective antimicrobial rinses for managing gingivitis. Over-the-counter options containing cetylpyridinium chloride (CPC) or essential oils also show meaningful plaque reduction in clinical trials.
- Stay hydrated — saliva is the mouth's natural defense against bacterial overgrowth. Drinking adequate water and chewing sugar-free gum stimulates saliva flow.
Professional Care
- Schedule cleanings every six months — professional scaling removes tartar (calcified plaque) that cannot be removed with home brushing, no matter how diligent you are. Patients with active gum disease may need cleanings every three to four months.
- Get annual X-rays — bone loss from periodontitis is often not visible clinically until it is substantial. Radiographs detect early interproximal (between-tooth) bone changes before symptoms emerge.
- Don't skip the periodontal exam — at every checkup, a dentist or hygienist should probe each tooth at six points to measure pocket depths. This is the clinical gold standard for staging gum disease and monitoring progression or improvement.
When to See a Dentist Urgently
While all gum-related symptoms warrant a dental appointment, certain signs suggest you should seek care promptly rather than waiting for your next scheduled cleaning:
- A tooth that has become visibly loose or shifted in position
- Spontaneous bleeding from the gums — not just when brushing
- Pus or a swelling at the gumline or between teeth
- Severe or worsening bad breath despite thorough brushing and flossing
- Persistent jaw or gum pain
- A dental abscess (a painful, pus-filled pocket at the root or gum)
These symptoms may indicate active infection and require prompt evaluation. A dental abscess in particular can progress to a serious systemic infection if untreated.
Frequently Asked Questions
Key Takeaways
Gum disease is one of the most common and most preventable chronic conditions affecting adults worldwide — yet it remains dramatically undertreated because its early signs are easy to dismiss. Here is what to take away from everything covered above:
- The early signs of gum disease — bleeding when brushing, swollen or red gums, persistent bad breath — are never normal and always warrant attention
- Gingivitis is fully reversible with improved home care and a professional cleaning; waiting allows it to become something that is not
- The stages of gum disease progress from gingivitis to mild periodontitis to advanced periodontitis, with each stage causing more irreversible damage to bone and tissue
- Periodontitis warning signs include receding gums, tooth sensitivity, loosening teeth, and spontaneous gum bleeding — any of these requires prompt dental evaluation
- Smoking, uncontrolled diabetes, and poor oral hygiene are the strongest modifiable drivers of disease progression
- Daily flossing, proper brushing technique, and twice-yearly professional cleanings remain the most effective tools for both preventing and managing gum disease
- Because gum disease is often painless until advanced, regular dental checkups are the only reliable way to catch it early
If you noticed something in this article that sounds familiar — bleeding gums, teeth that look longer than they used to, or breath that won't improve — the right next step is straightforward: schedule a dental appointment and ask for a full periodontal evaluation. The earlier you act, the more options you have and the less treatment you will ultimately need.