OTC Hearing Aids vs Prescription: What's the Real Difference?
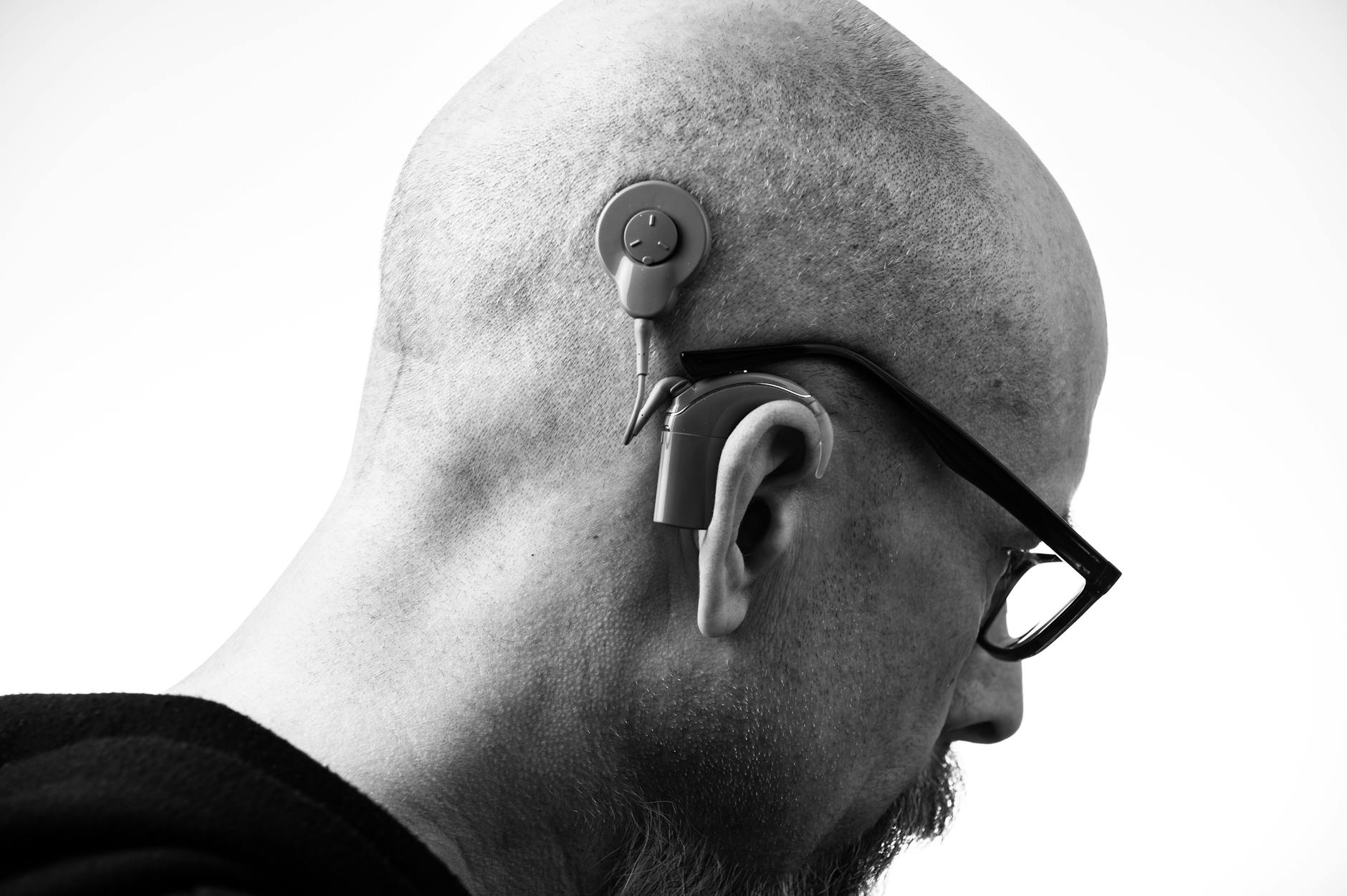
If you have been struggling to hear conversations clearly and wondering whether you actually need a $5,000 appointment with an audiologist, you are not alone. The question of OTC vs prescription hearing aids has become one of the most searched health topics in recent years — and for good reason. A landmark regulatory change in 2022 fundamentally shifted who can access hearing help and how much they should expect to pay for it.
This guide breaks down exactly what changed, who each type of device is designed for, what the real cost differences look like, and how to decide which path is right for your situation. No upselling, no pressure — just the facts you need to make an informed decision.
The 2022 FDA Rule Change That Changed Everything
For decades, hearing aids were classified as Class II medical devices in the United States, meaning they could only be sold through a licensed audiologist or hearing instrument specialist after a professional evaluation. That requirement was not just a formality — it was federal law, and it effectively put hearing aids out of reach for tens of millions of Americans who could not afford the full audiology pathway.
In October 2022, the U.S. Food and Drug Administration finalized a rule creating a new category of over the counter hearing aids — devices that adults with perceived mild to moderate hearing loss can buy directly, without a medical exam, prescription, or fitting appointment. The rule was years in the making, backed by research showing that self-fitting hearing aids perform comparably to professionally fitted devices for people with mild to moderate loss.
The practical effect was immediate. Major retailers including Walmart, CVS, Walgreens, Best Buy, and Amazon began stocking hearing aids on their shelves alongside reading glasses and blood pressure monitors. The average retail price dropped sharply, and brands like Sony, Jabra, Lexie, and Eargo entered the market with consumer-friendly products at accessible price points.
It was, by most assessments, one of the most significant consumer health policy changes of the decade. But it also created genuine confusion: do you need a prescription for hearing aids anymore, and if so, when?
Who Are OTC Hearing Aids Actually Designed For?
The FDA's OTC category has a specific intended user: adults 18 and older with perceived mild to moderate hearing loss. That phrasing — "perceived" — is deliberate. The rule does not require you to have a formal audiogram confirming your degree of loss. You are largely self-diagnosing based on your own experience.
Common signs of mild to moderate hearing loss that OTC devices are designed to address include:
- Difficulty following conversations in noisy environments like restaurants
- Frequently asking people to repeat themselves
- Turning up the TV louder than others find comfortable
- Missing parts of phone conversations
- Finding high-pitched sounds (doorbells, birds, alarms) harder to hear
- Mild tinnitus (ringing in the ears) accompanying the hearing difficulty
Mild hearing loss is typically defined audiologically as difficulty hearing sounds between 26 and 40 decibels. Moderate loss extends from 41 to 55 decibels. At these levels, self-fitted amplification with digital processing is often sufficient to meaningfully improve daily hearing.
The FDA rule explicitly excludes children under 18, and it strongly cautions against OTC devices for people with severe or profound hearing loss, sudden hearing loss, single-sided deafness, or hearing loss accompanied by pain, drainage, dizziness, or visible ear abnormalities. These conditions require professional medical evaluation and are not appropriate for self-treatment.
OTC vs Prescription Hearing Aids: A Side-by-Side Comparison
The differences between over the counter hearing aids and prescription devices go well beyond price. Here is a structured comparison across the factors that matter most.
Breaking Down the Real Cost of Prescription Hearing Aids
The sticker shock of prescription hearing aids cost is one of the main reasons so many people with hearing loss go untreated. The $3,000–$7,000 figure is not a rumor — it is confirmed by data from the Hearing Industries Association and multiple consumer health organizations.
What makes that price so high? Several factors:
- Professional services are bundled in. The quoted price almost always includes the audiological evaluation, the fitting appointment, follow-up programming visits over 1–3 years, and manufacturer warranty support. You are buying a package, not just hardware.
- The devices themselves are premium hardware. High-end prescription aids from Phonak, Oticon, Widex, and Starkey include sophisticated directional microphone arrays, AI-based sound classification, rechargeable batteries, and seamless Bluetooth streaming — technologies that genuinely outperform most OTC options.
- Distribution margins are substantial. Historically, hearing aids were sold exclusively through a small number of audiology practices with significant markups. The traditional dispensing model built high margins into the system.
It is worth noting that Medicare Part B does not cover hearing aids for most beneficiaries, though some Medicare Advantage plans include partial hearing benefits. Out-of-pocket costs remain the norm for the majority of people, which is precisely why the OTC category was such a meaningful change for middle- and lower-income households.
What You Give Up With an OTC Hearing Aid
The lower price and easier access of affordable hearing aids without prescription come with genuine trade-offs that are worth understanding clearly before you buy.
No Audiogram Means No Precision Fitting
The single biggest advantage of the prescription pathway is that your hearing aids are programmed to your specific audiogram — a graph of exactly how much amplification you need at each frequency across both ears. Your left ear may need more high-frequency boost; your right ear may have a different loss curve entirely. Prescription aids address this with clinical precision. OTC aids, even the best ones, work from a general amplification profile that you adjust yourself based on how things sound to you. For many people with mild loss, this is perfectly adequate. For others, it is noticeably less effective.
No Ongoing Professional Support
Hearing loss tends to change over time, and prescription devices come with built-in follow-up care. Your audiologist will reprogram your aids as your hearing changes, troubleshoot problems, and clean and repair the devices. OTC users are largely on their own — relying on app-based self-fitting tools and manufacturer phone support, which varies widely in quality.
Technology Ceiling
The very best prescription hearing aids — such as Phonak's Lumity or Oticon's Intent — use processing algorithms that are genuinely beyond what current OTC devices offer, particularly in complex listening environments with competing background noise. If your social or professional life involves a lot of group dinners, meetings, or events, the performance gap can be meaningful.
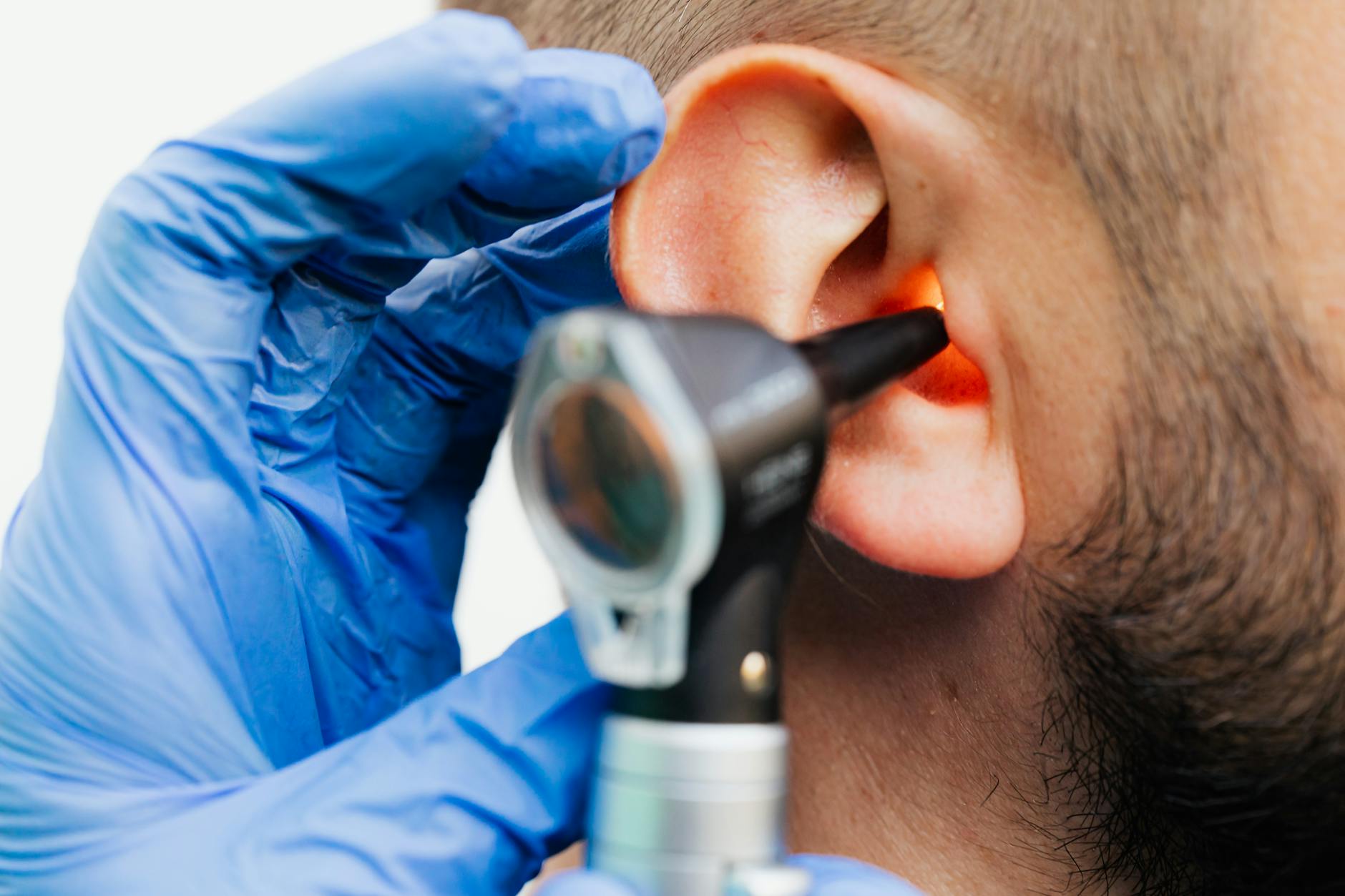
No Diagnostic Safety Net
Buying an OTC aid means skipping the medical evaluation that might catch a treatable underlying condition. Sudden hearing loss, asymmetric hearing loss (worse in one ear than the other), and hearing loss accompanied by tinnitus or dizziness can all signal conditions requiring medical treatment rather than amplification. An audiologist or ENT physician would catch these red flags; an app-based self-screening will not.
When Prescription Hearing Aids Are the Right Choice
The OTC category is genuinely useful, but it is not right for everyone. Here are the situations where the prescription pathway is the better — or only — medically appropriate option.
- Severe or profound hearing loss. If you struggle to hear even loud sounds, cannot understand speech even at close range, or rely on lip-reading significantly, you have loss that exceeds what OTC devices are designed to manage. You need a prescription device programmed to your specific audiogram.
- Sudden onset hearing loss. Hearing loss that develops over days or weeks rather than years is a medical emergency that requires prompt evaluation. It is not a situation to manage with a retail purchase.
- Asymmetric hearing loss. If one ear is significantly worse than the other, you need professional evaluation to rule out acoustic neuromas or other structural causes.
- Hearing loss in children or teenagers. The FDA's OTC category is for adults only. Any hearing loss in a person under 18 requires professional evaluation and prescription-grade devices.
- Hearing loss with associated symptoms. Ear pain, drainage, dizziness, a feeling of fullness in the ear, or visible abnormalities all require medical attention before any device is considered.
- When you have tried OTC and it is not enough. Many audiologists see patients who first tried an OTC aid, got partial benefit, and then came in for a professional evaluation. This is a perfectly reasonable two-step approach — try the accessible, affordable option first and escalate if needed.

Tips for Getting the Most Out of an OTC Hearing Aid
If you decide that the OTC route makes sense for your situation, a few practical steps will significantly improve your experience.
- Use the app-based fitting carefully. Most modern OTC aids come with a companion app that walks you through a brief hearing check and adjusts your device settings accordingly. Take this seriously — it is the closest thing to a professional fitting you will get, and rushing through it produces worse results.
- Give yourself an adjustment period. Wearing amplification for the first time is disorienting. Background sounds that your brain had been ignoring will suddenly be audible again. Most audiologists recommend wearing new aids for increasing periods over 2–4 weeks before concluding they are or are not working.
- Check the return window before you buy. Policies vary significantly — Best Buy typically offers 15 days, Amazon varies by seller, and some direct-to-consumer brands offer 45 or 60 days. A longer trial window gives you more time to accurately evaluate whether the device is meeting your needs.
- Keep an online hearing test in the loop. Several reputable organizations, including the American Speech-Language-Hearing Association, offer validated online hearing screeners. While these are not substitutes for a clinical audiogram, they can help you gauge whether your loss is in the mild-to-moderate range where OTC devices are appropriate.
- Get a professional check-up if you are not improving. If you have been using an OTC device consistently for 4–6 weeks and your hearing in key situations has not improved noticeably, that is a signal to see an audiologist. You may have more significant loss than you realized, or there may be a treatable underlying cause.
The Bigger Picture: Why Hearing Loss Treatment Matters
Untreated hearing loss is not merely inconvenient. Research published in journals including JAMA Internal Medicine and The Lancet has linked untreated hearing loss to accelerated cognitive decline, increased risk of dementia, depression, social isolation, and reduced earning potential. A 2023 study estimated that treating hearing loss early could reduce dementia risk by as much as 8 percent — a significant figure given the scale of dementia globally.
The barrier has historically been cost and access. The OTC rule change directly addresses both. Whether an individual ultimately goes the OTC or prescription route matters less than the decision to treat the loss in the first place. Millions of Americans who previously went without help now have a realistic, affordable path to better hearing — and that is an unambiguous public health win.
Final Verdict
The core answer to the OTC vs prescription hearing aids question is simpler than the marketing noise suggests: if you are an adult with mild to moderate hearing loss and no concerning associated symptoms, over the counter hearing aids are a legitimate, FDA-regulated option that will help most people at a fraction of the cost of the traditional audiology route. If your loss is severe, sudden, asymmetric, or accompanied by pain or dizziness, see a professional before buying anything.
The 2022 FDA rule change did not make prescription hearing aids obsolete — the professional pathway still offers clinically superior precision, ongoing support, and access to higher-end technology that genuinely matters for complex listening situations. What the rule change did do is give the tens of millions of people with untreated mild-to-moderate loss a practical first step that no longer requires a five-figure commitment to take.
The best hearing aid is ultimately the one you will actually wear. For many people, the most expensive option is not the most appropriate one — it is simply the one that existed before 2022.